Update transplant hospital definition
View commentsProposal Overview
Status: Implemented
Sponsoring Committee: Membership and Professional Standards (MPSC)
Strategic Goal: Promote living donor and transplant recipient safety
Policy notice 1/2017 (PDF - 195 K)
Board briefing 12/2016 (PDF - 160 K)
UNOS and OPTN member impact summary 12/2016 (PDF - 861 K)
Updates to how the OPTN defines a transplant hospital are needed to better describe attributes requiring consideration by the Membership and Professional Standards Committee (MPSC) when it reviews OPTN membership and transplant program designation applications. A transplant hospital member is currently defined by OPTN Bylaws as “a membership category in the OPTN for any hospital that has current approval as a designated transplant program for at least one organ” and by OPTN Policy as “a health care facility in which transplants of organs are performed.” A lack of distinguishing detail in these definitions has proven to be problematic when assessing the membership of healthcare institutional configurations consisting of multiple hospitals performing transplants of the same organ type at geographically separated sites. The goal of this proposal is to better define the basic accountable unit in which organ transplantation occurs so that meaningful, accurate, and conclusive assessments can be made regarding transplant program performance with patient safety, patient outcomes, and overall compliance with approved OPTN obligations.
Public comment: August 2016
Read the full proposal. (PDF - 154 K)
UNOS and OPTN member impact summary
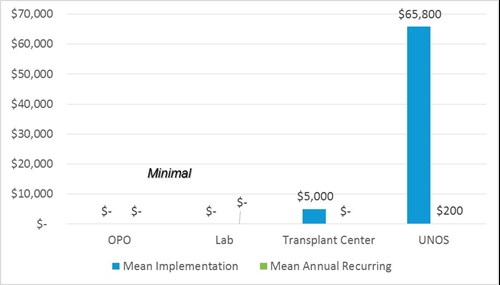
Project size/complexity
UNOS
Major implementation includes 600 hours in which member quality processes new forms from all transplant hospitals. Additionally, member quality and IT will work together to modify requirements in a system used to record and track memberships.
Project size = Large
Member
Transplant center
Implementation timeframe for transplant centers is minimal, estimated at three months for most centers. Time may be needed for staff to adjust any new or changed program criteria.
Existing workflow process, unique to each center, is the variable that most impacts implementation and ongoing financial resources. Additional staff time is needed to ensure patients meet all criteria for downstaging, exceptions, or listing. Small centers with fewer staff members may be most burdened, while larger centers may be able to more easily add additional staff hours and absorb financial impact.
Transplant center methodology notes
- One-time implementation cost impact estimate (for most transplant centers) of $5,000 is based on 40 hours of staff implementation time at a blended rate of $125/per hour. The rate includes administrators, doctors, and senior management.
- Recurring annual additional budget cost post-implementation is minimal, except for staff time in executing new or additional protocol.
- There is no cost savings.
OPOs and labs
OPOs and labs are not affected.
OPTN Policy/Bylaws affected
Bylaws Appendices
- D.2 (Designated Transplant Program Requirement),
- D.11.F (Veteran’s Administration (VA) Dean’s Committee Hospitals), and
- M (Definitions)
Summary of changes
There is now a list of characteristics to define what a transplant hospital is. The new definition allows members to perform transplants in more than one location, provided the locations meet the following requirements:
- Transplant ORs must have common executive leadership and governance oversight, demonstrated to satisfaction of the OPTN
- Transplant ORs must be preemptively documented with the OPTN
- Transplant ORs must also meet one of the following criteria:
1) Be within a “contiguous campus”
2) Be within a one-mile walking distance of the main hospital address
3) Be approved at the discretion of the OPTN
Under this new definition, only one member will be allowed per campus unless the other member is a children’s or Veterans Affairs (VA) hospital.
What Members Need to Do
After UNOS has completed necessary programming, it will provide notice to all transplant hospitals. Within 60 days of the notification, all transplant hospitals will be expected to notify UNOS of the transplant hospital’s intention to either remain recognized as the current, single transplant member; to separate its current membership into more than one transplant hospital member, or merge its existing membership with other existing transplant hospital members. In addition, all transplant hospitals will be expected to provide the following information:
- Type of campus arrangement (i.e., contiguous campus, one mile walking distance radius)
- Transplant operating room documentation, including:
- Maps that illustrate the transplant hospital campus and the location of each operating room facility
- Building name and address
- Floor number
- Unit identifier
No additional action is required of transplant hospitals that submit complete information and qualify as a single transplant hospital using either the “contiguous campus” or the “one-mile walking distance” geographical considerations.
Transplant hospitals with operating rooms beyond the established geographic boundaries may be asked to provide additional information for the MPSC’s consideration. The MPSC may also request that the transplant hospital participate in an informal discussion. During the discussion, the MPSC will expect the transplant hospital to explain their organization and why the MPSC should consider an exception to the explicit boundaries used to define a transplant hospital.
To allow transplant hospital members sufficient time to meet the new requirements, the OPTN will not implement the approved Bylaws definition for at least 12 months from the date UNOS provides notice to transplant hospital members.



